
Executive Summary: Community Mental Health Initiative Project Findings
CMHI 1.0 Building Systems of Care, Community by Community
Many Illinois communities have insufficient resources or strategies to address children’s healthy mental development. The Children’s Mental Health Initiative, Building Systems of Care, Community by Community (CMHI 1.0) was designed to enable four communities to find local solutions to these critical challenges.
Mental Health Disorder Prevalence
Population that will develop a mental health disorder at some point in their lifetimes
Of Those in US with Mental
Health Disorders
Of Those in US with Mental
Health Disorders
CMHI 1.0 Outcomes
With ILCHF grant funding, the four CMHI teams significantly shifted community culture and practices surrounding children’s mental health. CMHI has shown that empowering communities through an investment in their unique visions and capabilities enables providers to align their organizational plans and operations in order to more effectively serve children with a community-wide strategy.
- 4 communities have successfully integrated mental health systems across schools, primary healthcare and community organizations
- Services developed through the initial grant investment have been largely sustained
- CMHI 2.0, ILCHF committed $12.6 million to 5 new communities to build integrated systems for children’s mental health care
Children’s Mental Health Initiative 1.0
Children’s Mental Health Initiative 1.0
ILCHF Investment
$11.27 million
4 Communities
$2.85 million
Adams County Children’s Mental Health Partnership (ACCMHP), serving Adams County
$2.85 million
Community That Cares (CTC), serving Carroll,
Lee, Ogle, and Whiteside counties
$2.85 million
Livingston County Children’s Network (LCCN), serving Livingston County
$915,000
Cross-site evaluation
$2.85 million
The Children’s MOSAIC Project (MOSAIC), serving the city of Springfield
In 2009, ILCHF identified the following five guiding principles for CMHI:





8 Years
1 planning year
6 implementation years
1 mentoring year
Accomplishments & Lessons Learned
Every CMHI 1.0 community now incorporates the five guiding principles with varying levels of intensity and success.
ILCHF was committed to learning from and sharing the successes, challenges, and failures of each unique CMHI 1.0 project. To that end, each community wrote a manual describing its efforts, including problems, solutions, and strategies. The manuals are a rich resource of information about the extra- ordinary work in each community.
In synthesizing the key findings presented here, the Foundation draws upon extensive reports from the sites, third party evaluators, and ongoing relationships with key personnel at each site. Five primary elements of the projects discussed below are:
SYSTEMS INTEGRATION
CMHI 1.0 was very successful in significantly improving the level of systems integration in all four communities over the first six years of the project. Survey instruments sent to each service provider in the community provided ratings of all other providers in terms of their level of integration and partnership. Integration of human resources, funding, overall impact, and communication were assessed. The scale rated collaboration elements on a scale from one (informal relations) to five (full integration). All four communities achieved statistically significant improvement in their systems integration.
SUSTAINABILITY
CMHI 1.0 systems have been sustained, even as grant funding gradually decreased. From the onset of CMHI 1.0, ILCHF was concerned with sustaining enhanced mental health services and overall integrated systems of care beyond the grant period. All four communities utilized grant funds to pilot and implement the integration of mental health screening and services into both medical and school settings. These mental health services are now sustained through an array of funding mechanisms and strategies.
MENTAL HEALTH SCREENING
Mental health screening in schools and primary care practices are routine in all four CMHI communities. CMHI communities succeeded in dramatically increasing the rates of children being screened for developmental and mental health concerns. In 2010, at the start of the project, fewer than six percent of children were screened. By 2016, nearly half of all children in the communities were screened. In 2017, the Quincy Public Schools began screening all children during school registration. In 2018, Springfield public schools began screening all children in selected grades. For the CMHI communities, mental health screening is now routine for families and is part of the expected experience in medical care and school settings.
EVALUATION
CMHI incorporated a complex evaluation—including a cross-site evaluation and four local evaluations—producing varied but useful results. Systems integration data gathering produced useful results. The longitudinal cohort study encountered significant challenges in connection with enrolling and retaining children in the study, as well as difficulties in gathering data. These challenges have significantly informed the evaluation plan for CMHI 2.0.
ADVOCACY
Policy and advocacy capacity building was successful. ILCHF funded a collaboration between the CMHI 1.0 communities and the Sargent Shriver National Center on Poverty Law (Shriver Center). Shriver Center provided CMHI communities with technical assistance on policy advocacy, including the skills to navigate the Medicaid reimbursement system. The communities and Shriver Center worked together to devise education, legal advocacy, and problem-solving mechanisms that resulted in a significant strengthening of the children’s mental health system overall. The successes were primarily in the areas of insuring Medicaid reimbursement during the state budget impasse; expanding the available array of mental health services and increasing reimbursement rates; problem-solving around Medicaid coverage lapses for clients; and Medicaid plan changes.
Next Steps
Based on its experience with CMHI 1.0, ILCHF has learned that the most effective means of impacting the lives of children and families is to support the system of care at the community level. CMHI 1.0 produced impressive outcomes related to the successful integration of child-serving systems within the local community. CMHI 1.0 reduced the burden of emotional distress and mental illness. The services that were developed through the initial grant investment have been largely sustained.
ILCHF is committed to continuing its investment in the Illinois children’s mental health system: Children’s Mental Health Initiative 2.0 (CMHI 2.0) is a $12.6 million seven-year investment in a second round of system of care development grants. In July 2018, ILCHF awarded planning grants to five Illinois communities to develop and implement a children’s mental health system of care.
Children’s Mental Health Initiative Communities Served
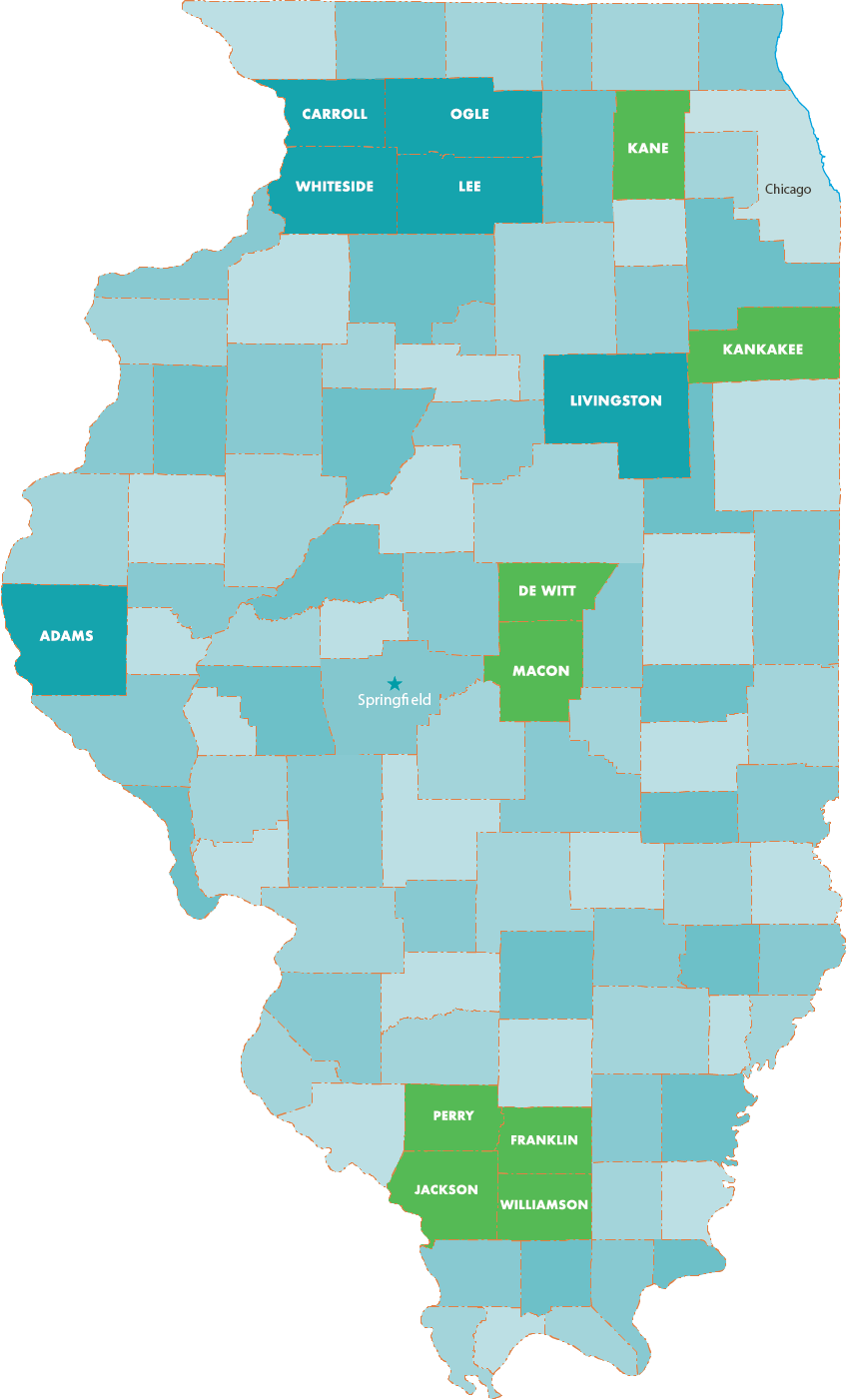
CMHI 1.0 Communities
- Adams County Children’s Mental Health Partnership (ACCMHP), serving Adams County
- Community That Cares (CTC), serving Carroll, Lee, Ogle, and Whiteside counties
- Livingston County Children’s Network (LCCN), serving Livingston County
- The Children’s MOSAIC Project (MOSAIC), serving City of Springfield
CMHI 2.0 Communities
- Centerstone, serving Perry, Franklin, Jackson, and Williamson counties
- Community Foundation of Kankakee River Valley, serving Kankakee County
- Heritage Behavioral Health, serving Macon and DeWitt counties
- Kane County Health Department, serving Kane County
- Primo Center for Women and Children, serving homeless youth and families in Chicago
Children’s Mental Health Initiative Timeline

September
- ILCHF releases Planning Grant RFP
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2010″ icon_replace=”true”]
May
- 13-month CMHI Planning Grants awarded to five communities
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2011″ icon_replace=”true”]
August
- Five-year grants awarded to four CMHI Communities
- Adams County
- Carroll, Lee, Ogle, and Whiteside Counties
- Livingston County
- City of Springfield
September
- Year one implementation begins
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2013″ icon_replace=”true”]
January
- Year two implementation begins
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2014″ icon_replace=”true”]
January
- Year three implementation begins
February
- ILCHF invests an additional year of funding of up to $300,000
for each community, to address unpredictable challenges in
systems change, thus adding a sixth implementation year
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2015″ icon_replace=”true”]
January
- Year four implementation begins
August
- CMHI Advocacy Planning Project Grant of $80,000 awarded to
Sargent Shriver National Center on Poverty Law (Shriver Center) - Advocacy Planning Project Grants of $5,000 each awarded
to the four CMHI communities
December
- Stabilization Grants of up to $175,000 each awarded
to the four CMHI communities
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2016″ icon_replace=”true”]
January
- Year five of implementation begins
October
- Advocacy Planning Project Grants of $5,000 each awarded
to the four CMHI communities
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2017″ icon_replace=”true”]
January
- Year six (final year) of implementation begins
August
- ILCHF Board authorizes up to $10.1 million for CMHI 2.0
planning, implementation, and evaluation
October
- Mentoring Grants of $75,000 each awarded to the four
CHMI communities
[/TS_VCSC_ProcessLines_Item][TS_VCSC_ProcessLines_Item timeline_style=”style4″ date=”2018″ icon_replace=”true”]
January
- Mentoring year begins
June
- CMHI 2.0 Planning Grants of $200,000 each awarded to
five new communities for planning, implementation, and evaluation
August
- CMHI Advocacy Planning Project Grant of $160,000 awarded
to Shriver Center
October
- CMHI 2.0 planning year begins
[/TS_VCSC_ProcessLines_Item][/TS_VCSC_ProcessLines_Container]
